|
||
|
||
|
||
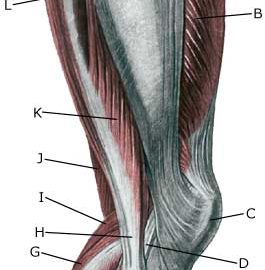
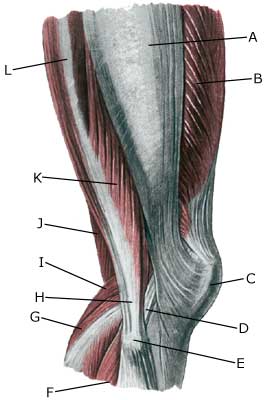
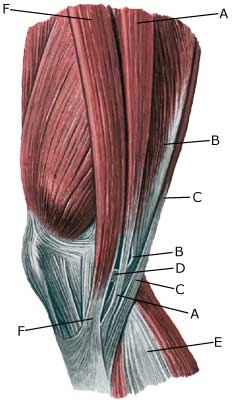
| Cause: Tendinitis occurs as a result of repeated uniform loads causing microscopic ruptures in the tendon, and especially at the tendon fastening, which causes an inflammation. Tendinitis is a warning that the exercise performed is too strenuous for the particular muscle tendons, and if the load is not reduced a rupture can occur (“pulled muscle”) or a chronic inflammation with a substantially longer rehabilitation period as a consequence.
Symptoms: Pain upon applying pressure along the tendon, aggravated when stretching or activation of the muscle tendon. Acute treatment: Click here. Examination: Medical examination is not necessarily required in slight cases. Severe cases or cases that are not improved by relief should be medically evaluated to ensure a precise diagnosis. The diagnosis is usually made on the basis of a normal medical examination, however, if any doubts surround the diagnosis an ultrasound scan can be performed as this is the best type of examination to ensure the diagnosis. Treatment: Relief, stretching and slowly increasing load within the pain threshold. If there is not sufficient progress with relief and regular rehabilitation, medical treatment in the form of rheumatic medicine (NSAID) or the injection of corticosteroid along the inflamed tendon can be considered. As the injection of corticosteroid is always a part of a long term rehabilitation of a chronic injury, it is often necessary for the rehabilitation period to stretch over several weeks to reduce the risk of relapse and ruptures. The tendon is naturally unable to accommodate maximum strain or load after a prolonged injury period after only a short rehabilitation period. If the diagnosis is made by use of ultrasound scanning and the injections are performed under ultrasound guidance, and the rehabilitation is progressed in accordance with the guidelines mentioned, then the treatment involving corticosteroid injections has very few risks connected. In cases of lack of progress with rehabilitation and medicinal treatment, surgery can be considered. However, this is very rarely necessary after a regular and strict rehabilitation period. The rehabilitation is dependant upon which tendons are involved, but it is usually the tendons in the popliteal space of the knee (tendons contributing to the flexing of the knee). Complications: If smooth progress is not achieved, it should be considered whether the diagnosis is correct or whether complications have arisen. Amongst others the following should be considered:
Special: Shock absorbing shoes or inlays will reduce the load. In case of lack of progress or recurrence after successful rehabilitation, a running style analysis can be considered to evaluate whether correction of the running style is indicated. |