|
||
|
||
|
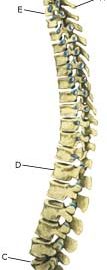
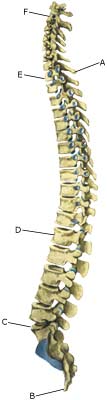
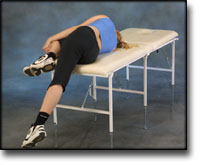
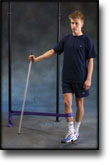
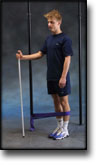
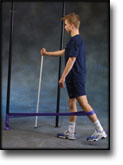
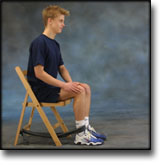
Cause: Scheuermann’s disease occurring in approximately 4% of the population (article). A curvature of the back occurs (bending over forwards) due to the vertebrae becoming wedge shaped. There are also characteristic x-ray finds. The cause of the condition is unknown, but evidence tends to suggest that the condition is hereditary (article). Symptoms: Back curvature localised high in the back (thoracal Scheuermann) gives often only few, if any, symptoms. Back curvature localised in the lower back (thoracolumbal or lumbal Scheuermann) does entail back pain for the majority (article). Treatment: The vast majority of cases can be treated with training, attempting to maintain the mobility of the back, counteract the curvature tendency and strengthen the stomach and back muscles. A corset can in some cases be used until the young person is fully grown. An operation can be performed only in very rare cases. The condition has a good prognosis (article), and even after an operation it is still possible to take part in many different forms of sport (article). Complications: In some cases a crooked back can have other causes (infection, nerve disease, inborn bone change, rheumatic illness, bone disease, metabolic disorder). |