|
Metacarpal and phalangeal fractures in athletes. |
Kategoriarkiv: Arm
Treatment
|
Complications of plate fixation in fresh displaced midclavicular fractures. METHODS. RESULTS. CONCLUSIONS. |
Treatment(3)
|
Displaced supracondylar fractures of the humerus in children. Audit changes practice.
|
Treatment(2)
|
Elbow injuries in childhood.
|
Treatment(1)
|
The management of forearm fractures in children: a plea for conservatism.. |
Examination
|
Elbow effusions in trauma in adults and children: is there an occult fracture? |
Complications
|
Hyperextension injury to the PIP joint or to the MP joint of the thumb–a clinical study. |
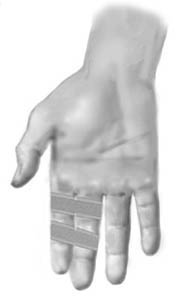
tape-instruction
Objective: Stabilise finger joints. |
|||
 |
|||
| Application: Two anchor strips are applied, one on each side of the affected joint on the finger. Strips are similarly applied to the neighbouring finger. The two fingers are subsequently taped together with strips on the anchors. The healthy finger can in this manner stabilise the injured finger, whilst both fingers can still be bent and stretched. |
Treatment(3)
|
Early active mobilisation of volar plate avulsion fractures. |
Treatment(2)
|
Role of MR imaging in the management of “skier’s thumb” injuries. |
