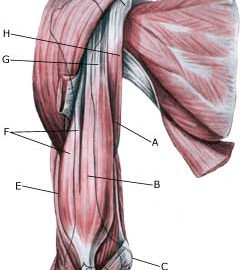
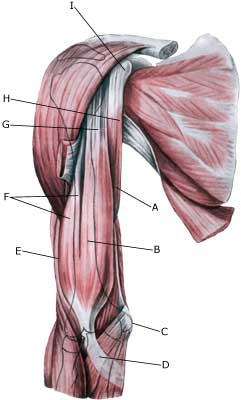
INFLAMMATION OF THE BICEPS TENDON
|
||
|
||
| Cause: In case of repeated (over)loading (swimming, throwing) the long head of the biceps muscle (caput longum biceps bracii) becomes inflamed. Inflammation of the biceps tendon is also called a “swimming shoulder”. In some cases fluid is formed in the tendon sheath on the front of the upper arm (tenosynovitis). Inflammation of the biceps tendon is very often seen in conjunction with other damage in the shoulder, such as: impingement syndrome, inflammation of the upper shoulder blade muscle, rupture of the upper shoulder blade muscle, inflammation of the bursa (bursitis subacromialis), meniscus lesion in the shoulder (laesio labrum glenoidale). With age and repeated loads the biceps muscle becomes marked by wear and tear, which increases the chance of ruptures. Ruptures occur most often when the muscle is contracting while being stretched (eccentric contraction). Long-term inflammation of the tendon sheath (tenosynovitis) increases the chance of a rupture of the tendon. It is rare for healthy tendons to rupture. Symptoms: Slowly insetting localises tenderness exterior and to the front of the shoulder after load. Sometimes radiating down the upper arm. Pain deteriorates, when external pressure is applied to the biceps tendon, the front of the shoulder, when the muscle is activated (attempting to bend the arm against resistance) and when the muscle is taut (stretching and at the same time rotating inwards in the elbow (pronating)). Acute treatment: Click here. Examination: In light cases with only minimal tenderness medical examination is not necessarily required. In case of more pronounced pain and in lieu of progress a medical examination should be carried out to ensure the correctness of the diagnosis and to commence the correct treatment. Ordinary medical examination is often sufficient to form the diagnosis, but if uncertainty exists, it should be supplanted by ultrasound, which is the most suited examination for shoulder injuries (article) (Ultrasonic image). Treatment: The treatment consists of relief and slow rehabilitation of the biceps muscle and the other muscles around the shoulder. Only in cases of total rupture of the biceps muscle should surgery be considered, the vast majority are treated with rehabilitation. If no progress is made with relief of the tendinitis, medical treatment may be considered in the form of rheumatic medicine (NSAID) or draining of the fluid in the tendon sheath and injection of corticosteroid in the tendon sheath, which must be performed with ultrasound guidance. Since the injection of corticosteroid is part of a long-term rehabilitation of a long-term injury, it is often necessary that the rehabilitation period stretches over several weeks, to reduce the risk of recurrences and ruptures. Naturally the tendon can not sustain maximum load after only a short rehabilitation period. Complications: If smooth progress is not achieved the correctness of the diagnosis, or whether complications have arisen should be considered. Amongst others the following should be considered:
…and ailment inside the shoulder (the fluid in the biceps tendon may be from the shoulder joint). |