RUPTURE OF THE BICEPS TENDON
|
||
|
||
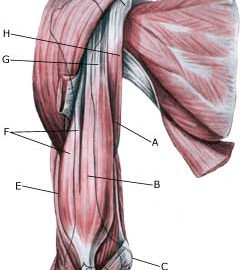
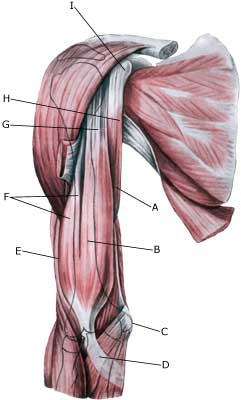
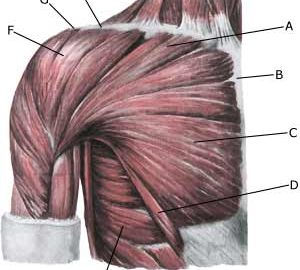
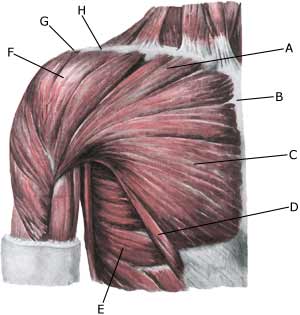
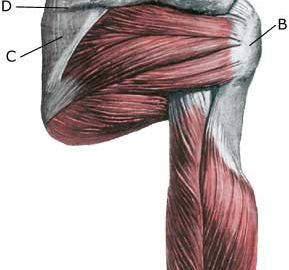
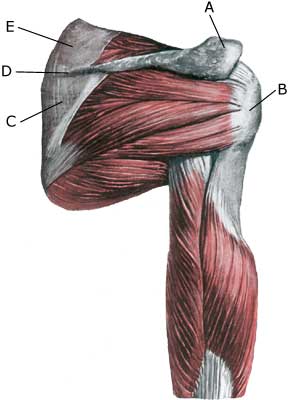
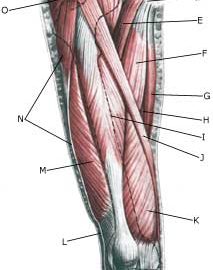
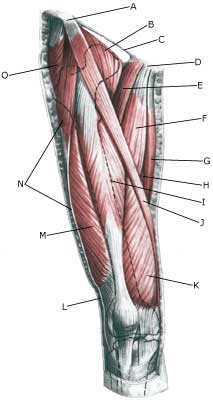
| Cause: A rupture of the biceps muscle (caput longum) often occurs due to changes in the tendon due to wear and tear following many years’ repetitive load or attributable to a single violent load (for example weight lifting). Ruptures occur most often when the muscle is contracting while being stretched (eccentric contraction). Long-term inflammation of the tendon sheath (tenosynovitis) increases the chance of a rupture of the tendon. It is rare for healthy tendons to rupture.
Symptoms: Sudden insetting localised tenderness exterior and to the front of the shoulder after load. Sometimes radiating down the upper arm. Pain is aggravated when external pressure is applied to the biceps tendon, the front of the shoulder, when the muscle is activated (attempting to bend the arm against resistance) and when the muscle is taut (stretching and at the same time rotating inwards in the elbow (pronating)). A swelling can often be observed (the contracted biceps muscular belly) above the bend of the arm (cubital fossa). Acute treatment: Click here. Examination: In case of sudden insetting pain and swelling above the elbow a medical examination should be carried out to ensure the correctness of the diagnosis and to commence the correct treatment. Normal medical examination is often sufficient to form the diagnosis, but if any doubts exist the examination should be supplemented by an ultrasound scan, which is the most suited examination for shoulder injuries (article) (Ultrasonic image). Treatment: The treatment consists of relief and slow rehabilitation of the biceps muscle and the other muscles around the shoulder. Only in cases of total rupture of the biceps muscle should surgery be considered, as the vast majority of ruptures are treated with rehabilitation. Complications: If smooth progress is not achieved the correctness of the diagnosis should be considered, or whether complications have arisen. Amongst others the following should be considered:
…and pain inside the shoulder (the fluid in the biceps tendon may emanate from the shoulder joint). |